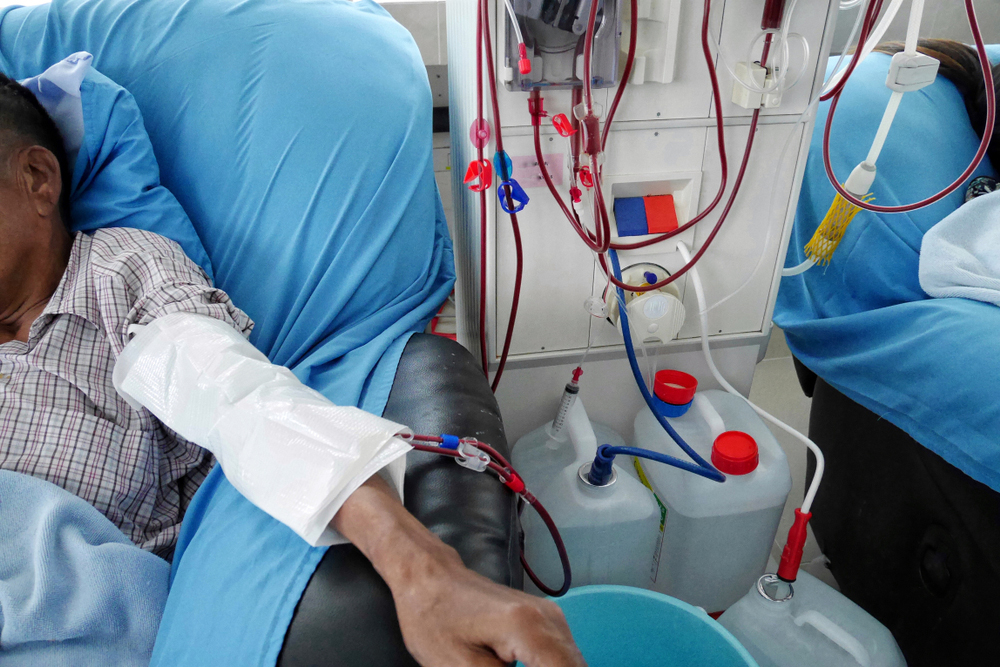
The Union health ministry has decided to provide peritoneal dialysis, a home-based alternative to haemodialysis that typically requires thrice weekly hospital visits, to patients with end-stage kidney disease across India under the National Dialysis Programme.
It will be available free to below-poverty-line patients and at a cost to the rest, just as haemodialysis is under the NDP.
The ministry has sent guidelines to the states and Union Territories, urging them to train staff and ensure the patients receive the special fluid used in peritoneal dialysis.
Nephrologists say peritoneal dialysis is a more attractive and less risky option for patients than haemodialysis.
In peritoneal dialysis, the peritoneum — the membrane lining the cavity of the abdomen and covering the abdominal organs — is used to filter wastes and excess water from the blood.
A catheter delivers the special dialysate fluid into the belly, where it absorbs the wastes and extra fluid from the blood and drains out into an empty bag.
This is done two or three times a day, with the catheter permanently in place, and the patient has to periodically empty the bag in which the waste collects.
Health-care workers need to visit the patients at their home just once to insert the catheter and instruct them on how to carry out the self-dialysis.
Research suggests that home-based self-dialysis carries a lower risk of infection than the twice or thrice-a-week dialysis sessions in clinics or hospitals.
Haemodialysis services under the NDP, launched in 2016, are available through 765 clinics in 444 districts, delivered through over 4,400 machines. But haemodialysis remains hard to access for the large numbers of patients who have no dialysis centres near their homes.
The ministry has asked the states to set up panels led by nephrologists at government hospitals to oversee the introduction of peritoneal dialysis.
“This is a major decision that could improve the quality of life of patients,” said senior nephrologist Vivekanand Jha, executive director of The George Institute of Public Health, New Delhi, and chair of an expert panel that had recommended the health ministry introduce peritoneal dialysis into the NDP.
Although the technology has been available for nearly two decades, peritoneal dialysis has not become popular in India. Health experts estimate that about 225,000 people across the country develop end-stage kidney disease each year, typically the outcome of uncontrolled diabetes or high blood pressure.
The number of patients on dialysis is estimated to range between 75,000 and 100,000. Only about 6,500 of them are estimated to be on peritoneal dialysis.
Jha and other doctors have been concerned that peritoneal dialysis is not even offered to patients as an option.
“Haemodialysis means repeated visits to clinics or hospitals and opportunities for nephrologists to earn money. There’s been a bias away from peritoneal dialysis in the private sector,” Jha said.
Nephrologists who were part of the expert panel said that peritoneal dialysis had been misleadingly labelled as more expensive than haemodialysis.
They say that haemodialysis, which costs a paying patient about Rs 2,600 a session at a public hospital, is comparable in cost or more expensive than peritoneal dialysis, depending on the number of dialysis sessions per week.
In peritoneal dialysis, the one-time spending on the catheter-related devices comes to about Rs 10,000, while the dialysate solution currently costs Rs 15,000 to Rs 20,000 a month. For most patients, peritoneal dialysis would be the less expensive option, said Tarun Jeloka, a Pune-based senior consultant nephrologist.
“Local manufacture and the promotion of peritoneal dialysis on a large scale through the National Dialysis Programme would help lower the costs,” Jha said.
Nephrologists are hoping that the government’s decision to introduce peritoneal dialysis in the NDP would expand the use of the option in the private sector too.
“We’ve recommended self-care tools to help people on peritoneal dialysis lower the risk of complications by detecting them early and remaining in touch with health-care providers,” said Narayan Prasad, secretary-general of the Indian Society of Nephrology.