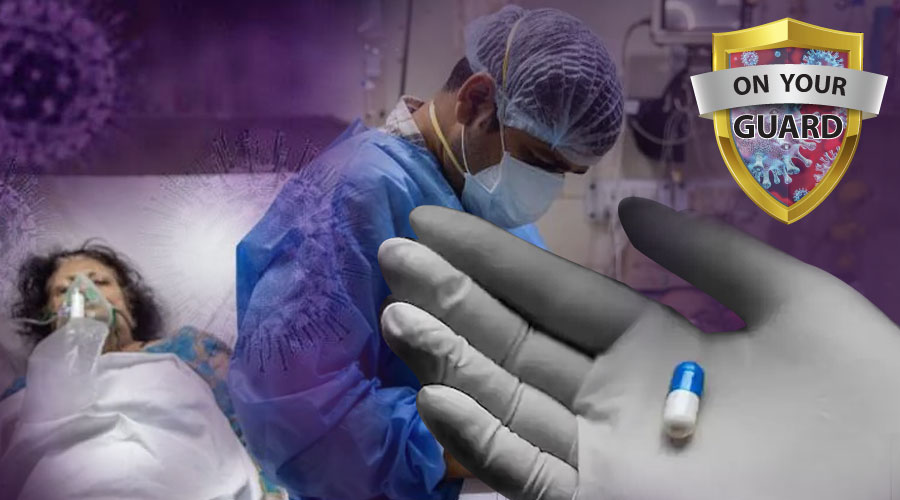
As Spiralling Covid cases continue to wreak havoc through the country, overwhelming the health infrastructure, a new threat has appeared on the scene in the form of “black fungus” which in its most aggressive form affects the eyes, nose and at times the brain of vulnerable patients.
Maharashtra has attributed several deaths to black fungus or “mucormycosis” with the state government apprehending that there could be as many as 2,000 patients with varying degrees of infection. Early this week, Odisha reported its first black fungus case, while Delhi, Gujarat, Andhra Pradesh, Karnataka, and Jharkhand have already identified cases.
The situation is serious enough for the Union health ministry to issue an advisory (May 9) for screening, diagnosis and management of mucormycosis infections.
What exactly is this disease? Mucormycosis, or zygomycosis, is a critical fungal infection that is caused by a group of molds (a type of fungus) known as mucormycetes, according to the CDC or Centers for Diseases Control and Prevention in the US.
Molds are already present in the environment — soil, plants, manure and decaying fruits and vegetables. Mucormycosis, spotted throughout the world, can be acquired in hospitals, most commonly by vulnerable transplant patients, when the molds get on hospital linen and/or travel through ventilation system.
The infection attacks people with comorbidities or weak immunity. Thus, those who recuperate from Covid-19 but have comorbidities — such as diabetes, kidney infection, heart disease, or cancer — are the most vulnerable.
So why is it appearing now in India, which is in the midst of a deadly second wave of coronavirus infections? According to Peter Collignon, who is a member of the WHO expert committee on antibiotic resistance and infectious diseases, Covid-19 was creating conditions for the infection to take hold. People’s immune systems were being compromised by the virus. “We give a lot of high-dose steroids now to people with Covid-19 if they end up in intensive care as the steroids help to treat inflammation, but the steroids unfortunately also suppress your immune system… So that’s why we don’t like giving steroids to patients longer than we absolutely have to.”
The infection can be life-threatening in diabetic or severely immune-compromised patients. In its May 9 advisory, the Centre said that black fungus mainly affects people who are on “medication that reduces their ability to fight environmental pathogens”. According to the Indian Council of Medical Research (ICMR), “Mucormycosis, if uncared for, may turn fatal. Sinuses or lungs of such individuals get affected after fungal spores are inhaled from the air.”
The first signs of black fever are face numbness, swelling in the eyes, and nose obstructions on one side, nasal discharge (blackish/bloody), loosening of teeth, shortness of breath, bloody vomits, altered mental status, chest pain, gastrointestinal bleeding and abdominal pain, among others.
Doctors suggest that vital parameters like blood glucose level, oxygen level etc of vulnerable patients should be monitored regularly after they recover from Covid-19. Steroids should be used judiciously in correct timing, dosage and duration; clean sterile water should be used in humidifiers during oxygen therapy; and antibiotics and antifungal medicines should be used correctly.
The fatality rate is high in black fungus infections as most patients come for medical care only after the symptoms intensify.
Amphotercin-B is being used as the key medicine in treating black fungus patients in India. The other option is to administer a dose of anti-fungal intravenous injection (costing Rs 3,500 per jab) every day for about two months. Some cases of mucormycosis may eventually require surgery.
PS: The recommendations in this column (source: Union ministry of health and family welfare, CDC, WHO) are intended as general advisories. For specific concerns, especially for those with comorbidities, it is advisable to consult your family physician.