Nearly three decades ago our world was first referred to as a “global village” but we never realised that this connection between the countries could be so strong until last year when the Covid-19 pandemic broke out and the virus started engulfing countries one after another, exposing the health systems of even many developed nations.
The pandemic has forced us to think about the condition of the healthcare system and preparedness for any such adversity worldwide. The inadequacies in coping with any medical emergency have been exposed and the scarcity of essential infrastructure, medicines and logistics is starkly visible now.
India has a huge and dense population, which has led to insufficient testing, delayed reporting, scarcity in supply of drugs, non-availability of medical oxygen and the tardy vaccination drive.
Only the over-stressed frontline Covid warriors are courageously fighting the deficiencies at the cost of their own lives.
As far as Bihar is concerned, the situation might turn grimmer because the health system of the state is a matter of concern. Of the total population, 89 per cent resides in the rural areas and has less access to health facilities. So, if the infection spreads uncontrollably in the villages, the situation may turn worse.
We have to look into history to understand the circumstances better. Bihar has suffered discrimination since the colonial period, which continued even after Independence.
Bihar is a land-locked state and does not have any port city of its own. All the economically viable agro-products and mineral resources were drained out systematically. The prevalence of the zamindari system, the policy of freight equalisation after Independence and the bifurcation of Bihar and Jharkhand in 2000 have led to the downfall of the economy of Bihar.
Geographically too, Bihar is at a disadvantage. It is the only state whose northern region witnesses floods while the southern region reports draughts at the same time almost every year. Even after the concerted efforts of governments, Bihar’s per capita income of Rs 31,287 remains the lowest among the major states and is 32.9 per cent lower than the national average.
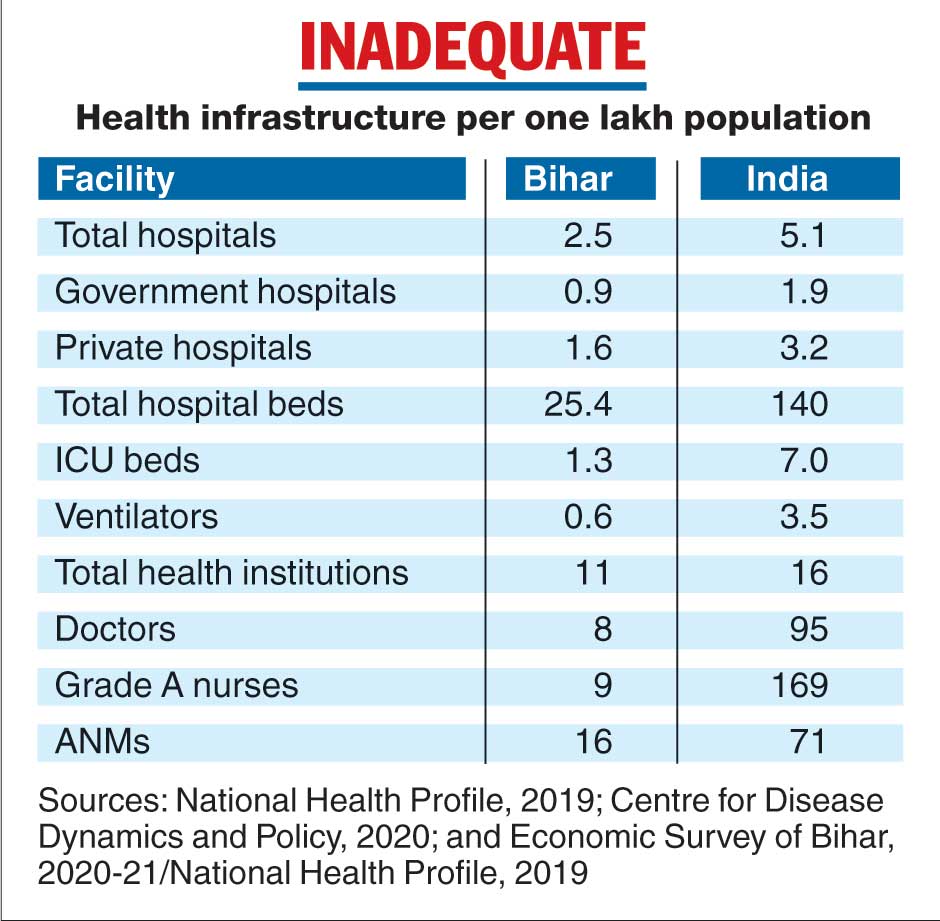
Health infrastructure
As per Census 2011, Bihar has a population of 10.4 crore. According to the Bihar Economic Survey (BES) 2020-21, the state has 12,023 health institutions, 9,842 doctors, 10,594 Grade-A nurses and 19,861 auxiliary nursing midwifery (ANM) workers. When provisioning for clean drinking water and sanitation alone is a challenging task, the lacunae in the health sector are somewhat expected.
According to the state health department, Bihar had reported a total of 6.92 lakh Covid-19 cases till May 24. Of these, 6.5 lakh have recovered and 4,642 deaths recorded.
The recovery rate is 93.85 per cent.
Despite numerous adversities, the state created 546 isolation centres with 56,490 beds, of them 4,552 with oxygen support. Along with ramping up testing, initiatives like the appointment of health staff and the creation of community kitchens have been initiated. Till May 25, 80.42 lakh people had got the first dose of vaccine and 19.43 lakh were fully vaccinated.
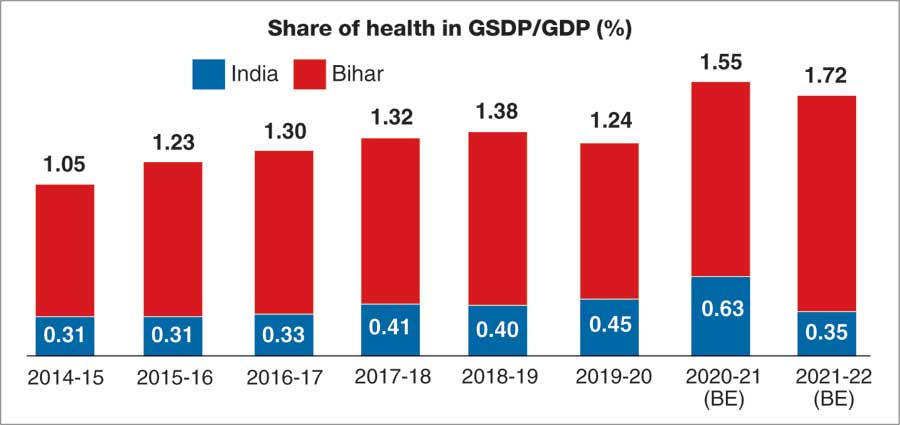
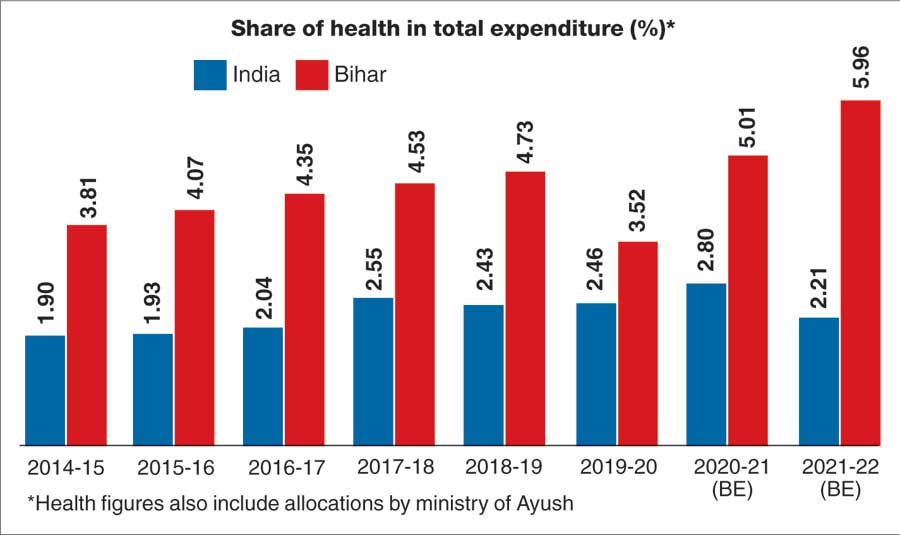
Expenditure on health
The pandemic has exposed the under-funding in the social sector. To set things right, the 15th Finance Commission had recommended that the Centre increase public spending on health to 2.5 per cent of the GDP by 2025 while the states ramp up health funding to more than 8 per cent of their budget by 2022.
The commission had recommended grants-in-aid of Rs 1,06,606 crore to the health sector, of which Bihar had been earmarked Rs 10,740 crore. The health sector has already been suffering from issues such as weak infrastructure, human resource scarcity and excess out-of-pocket-expenditure (OoPE).
Covid-19 has worsened the scenario. About 70 per cent of Bihar’s revenues come from central transfers. The state has always tried to get its allocation on health increased but health spending has been showing a declining trend in the country.
The share of health spending in the GDP is around 0.40 per cent for India and 1.35 per cent for Bihar.
According to the ministry of health and family welfare, the OoPE per hospitalised case excluding childbirth in Bihar is Rs 11,182 in rural areas and Rs 23,647 in urban areas.
Private hospital charges are Rs 15,220 in rural areas and Rs 32,319 in urban areas, according to National Health Systems Resource Centre figures from 2014.
According to the BES, the in-patient occupancy rate in government hospitals of Bihar is only 55 per cent.
Although Bihar’s expenditure on health is around 4 to 5 per cent, the public sector has not been able to deliver the services as per the requirement, which leads to high OoPE that is a great burden on people where the poverty line for a person was fixed at Rs 778 per month for rural areas and Rs 923 for urban areas (2011-12).
The country is passing through an unprecedented crisis. The state and central governments should work in harmony to deal with the situation.
In a state like Bihar where health facilities are mainly concentrated in Patna or in a few other district towns, efforts must be made to strengthen the structure in other districts and blocks. Private hospitals should also be encouraged to take up responsibilities.
To control unbridled hospitalisation in the private sector, all healthcare charges must be regulated and rationalised by the government.
As per the 7th Schedule, health comes under the State List but the responsibilities of this sector are immense, so it should be shifted to the Concurrent List.
Nabarun Ganguli is the director of the ONOH Foundation, Bihar. Barna Ganguli is assistant professor, CEPPF, ADRI. The ONOH Foundation works on health in Bihar and Jharkhand