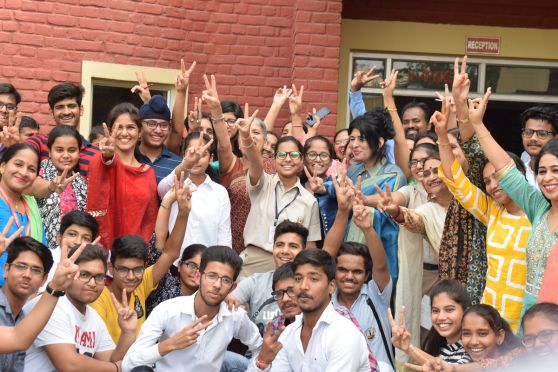Monday, 06 May 2024
Monday, 06 May 2024
 Monday, 06 May 2024
Monday, 06 May 2024








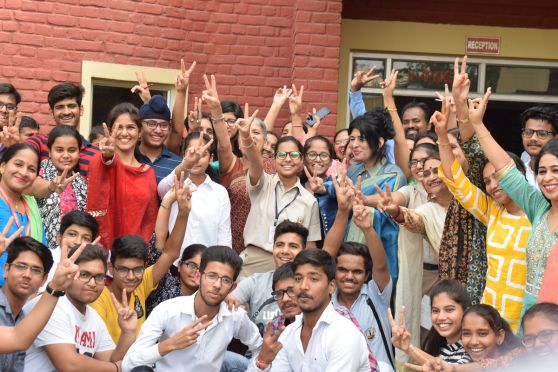







Gear up for Baahubali’s animated spin-off
The second season of ‘Nikhoj’ is officially underway
Get trendy with this Ayushmann Khurrana-approved lifestyle brand
Don’t miss Nussrat Jahan’s hilarious attempt at using chopsticks
Beat the heat with chef Kunal Kapur’s Rose Mojito recipe
Let us reflect on some hard realities of contemporary India. ‘Mere’ corruption is no longer an electoral issue: we do not shun politicians because they might have their hands in the till or in our pockets
SUKANTA CHAUDHURI

Epidemic Plan, envisioned as a collaborative endeavour among the Central govt, state governments, and relevant stakeholders, aims to provide a comprehensive blueprint for coordinated action
BASIL GUPTA
The attitude of the West to its Muslim citizens is beginning to mirror their hostility towards non-client Muslim states abroad. Some of this is a hangover of the ‘war on terror’ since 9/11
MUKUL KESAVAN
The ideological penetration of Indian science by Hindutva was starkly illustrated by a series of nine linked tweets issued by the secretary of the department of science and technology last month
RAMACHANDRA GUHA
Tapping into the state’s economic potential must also be a representative process. Unity, rather than uniformity, should be the preferred goal while restoring normalcy to Manipur
THE EDITORIAL BOARD






















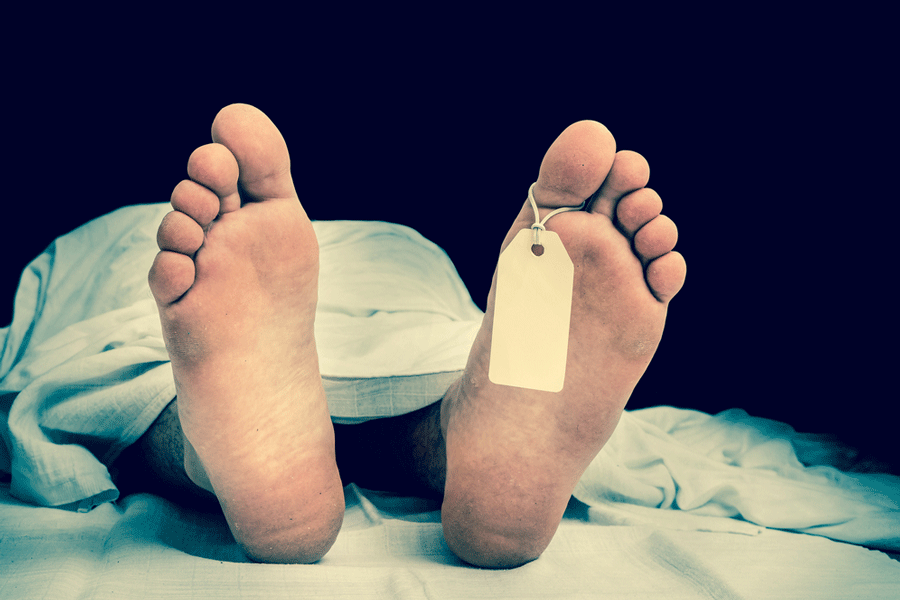








Directed by Chidambaram S. Poduval, the survival thriller is currently streaming on Disney+ Hotstar